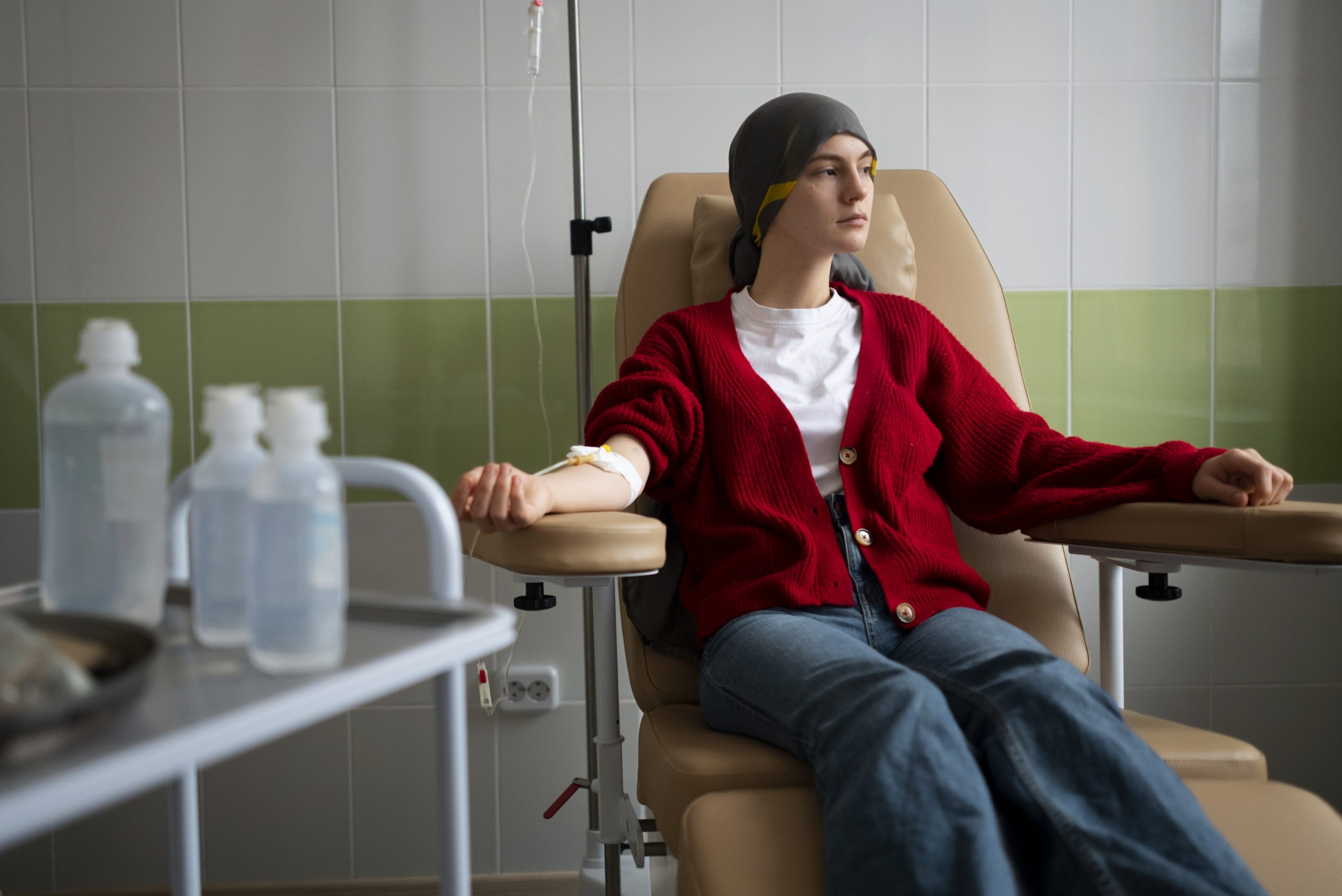

According to a recent study, inflammation levels that indicate poor survival chances are two to three times more likely to be present in lung cancer patients with moderate to severe depression.
The findings could shed light on why a sizable fraction of lung cancer patients do not respond to modern immunotherapy and targeted therapies, which have greatly extended survival for many lung cancer patients.
“These patients with high levels of depression are at much higher risk for poor outcomes,” said Barbara Andersen, one of the lead authors of the study and professor of psychology at The Ohio State University. “Depression levels may be as important or even more important than other factors that have been associated with how people fare with lung cancer.”
In the journal PLOS ONE, the study was only just published online.
Andersen and associates at The Ohio State University Comprehensive Cancer Center—Arthur G. James Cancer Hospital and Richard J. Solove Research Institute at Ohio State University examined 186 patients who had just received an advanced lung cancer diagnosis (Stage IV). They were curious about the relationship between systemic inflammation ratio (SIR) biomarker levels at diagnosis and depression levels.
Three biomarkers linked to inflammatory processes in the body are included in SIRs. Greater inflammatory levels are riskier and are associated with decreased survival rates.
A depression assessment was also completed by each individual. The findings revealed that 35% of patients experienced moderate to severe depression symptoms.
“Of all cancer patients, those with lung cancer are among those with the highest rates of depression, which makes the findings of our study even more concerning,” Andersen said.
The crucial result, according to Andersen, was that patients with the highest degrees of depression were driving the link between higher depression scores and higher inflammatory ratings.
Take one of the study’s biomarkers, the platelet-to-lymphocyte ratio, as an illustration. 56% of patients had levels of inflammation that were dangerously high compared to 42% who had mild or no symptoms of depression.
Nevertheless, only 23% of people who had modest levels of inflammation and 77% of people with high levels of depression fell below the threshold.
“It was patients with high depression levels who had strikingly higher inflammation levels, and that is what really drove the correlation we saw,” she said.
Even after adjusting for other variables associated to inflammation biomarker levels, such as demographics and smoking status, these severely depressed patients still had a 1.3–3 fold increased risk of having high inflammation levels.
Also, studies had revealed that all three biomarkers’ initial levels predicted overall survival. Those with increased neutrophil-to-lymphocyte ratios, one of the inflammatory indicators, had a roughly doubled risk of passing away at any moment during the following two years compared to individuals with lower inflammation ratios.
Andersen pointed out that this study examined the relationship between depression and inflammation in newly diagnosed, untreated patients.
However, controlling for depression levels upon diagnosis, Andersen and her colleagues showed that the trajectory of persistent depression symptoms over time predicted survival in a prior study. This was the first investigation into the danger to survival posed by persistent depressed symptoms during and after treatment.
According to Andersen, the mounting evidence points to the significance of assessing and managing depression in lung cancer patients.
She pointed out that in this study, individuals with high depression and elevated inflammation predominated over those with other factors linked to a poorer chance of surviving cancer, such as low educational attainment, being overweight, and performing poorly on a test of daily functioning.
Some medical professionals might believe that cancer patients’ depression is typical, however she said it’s not true.
“It is normal to be upset, sad and anxious about a cancer diagnosis, but it is not normal to have major depression,” Andersen said.
“Depression should not be discounted. This study shows the strong link between depression and inflammation, with both related to poor outcomes.”
more recommended stories
 Nanoplastics in Brain Tissue and Neurological Risk
Nanoplastics in Brain Tissue and Neurological RiskKey Takeaways for HCPs Nanoplastics are.
 AI Predicts Chronic GVHD Risk After Stem Cell Transplant
AI Predicts Chronic GVHD Risk After Stem Cell TransplantKey Takeaways A new AI-driven tool,.
 Red Meat Consumption Linked to Higher Diabetes Odds
Red Meat Consumption Linked to Higher Diabetes OddsKey Takeaways Higher intake of total,.
 Pediatric Crohn’s Disease Microbial Signature Identified
Pediatric Crohn’s Disease Microbial Signature IdentifiedKey Points at a Glance NYU.
 Nanovaccine Design Boosts Immune Attack on HPV Tumors
Nanovaccine Design Boosts Immune Attack on HPV TumorsKey Highlights Reconfiguring peptide orientation significantly.
 High-Fat Diets Cause Damage to Metabolic Health
High-Fat Diets Cause Damage to Metabolic HealthKey Points Takeaways High-fat and ketogenic.
 Acute Ischemic Stroke: New Evidence for Neuroprotection
Acute Ischemic Stroke: New Evidence for NeuroprotectionKey Highlights A Phase III clinical.
 Statins Rarely Cause Side Effects, Large Trials Show
Statins Rarely Cause Side Effects, Large Trials ShowKey Points at a Glance Large.
 Anxiety Reduction and Emotional Support on Social Media
Anxiety Reduction and Emotional Support on Social MediaKey Summary Anxiety commonly begins in.
 Liquid Biopsy Measures Epigenetic Instability in Cancer
Liquid Biopsy Measures Epigenetic Instability in CancerKey Takeaways Johns Hopkins researchers developed.

Leave a Comment