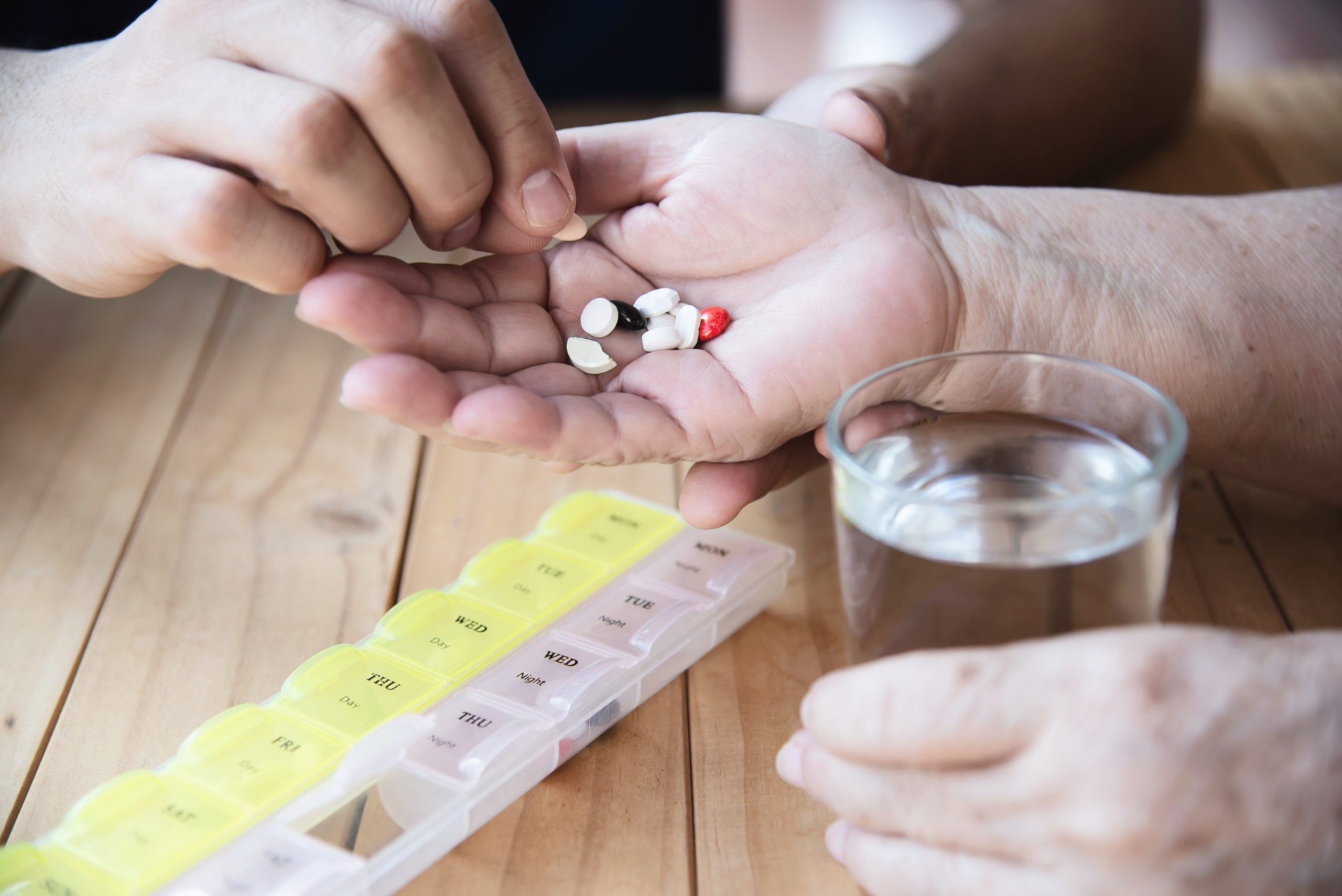

According to a new RAND Corporation study, states that seek to boost access to buprenorphine, a lifesaving drug used to treat opioid use disorder, should explore initiatives to improve professional education and clinician expertise.
Researchers examined six state-level policies aimed at increasing buprenorphine use and discovered that requiring buprenorphine prescribers to receive additional education beyond the initial required instruction, as well as continuing medical education related to substance abuse, were both associated with a significant increase in treatment use.
The findings were published in the most recent issue of JAMA Health Forum.
“Many studies suggest that physicians and other health providers are apprehensive about whether they have sufficient knowledge about using buprenorphine to treat opioid use disorder,” said Bradley D. Stein, the study’s lead author and a physician scientist at RAND, a nonprofit research organization. “We found that requiring additional ongoing education seems to help address this worry, empowering them to make greater use of their training.”
The study looked at the effects of six different state-level policies: rules requiring additional education for buprenorphine prescribers beyond the initial X-waiver training; continuing medical education related to substance misuse and addiction; expanding Medicaid coverage to include buprenorphine treatment; mandating prescriber use of prescription drug monitoring programs; and regulating pain management clinics.
The frequency of fatal opioid overdoses in the US continues to rise, and an estimated 5.6 million people in the country suffer from an opioid use disorder. Medication treatment for opioid use disorder is regarded the gold standard of care, enhancing quality of life and lowering the rate of fatal overdoses.
The new study used data from 90% of prescriptions filled at retail pharmacies in the United States to identify buprenorphine prescriptions filled between 2006 and 2018. The researchers utilized a range of sources to determine when states introduced any of the six policies under consideration.
The records were evaluated to identify new episodes of buprenorphine treatment for opioid use disorder, comparing trends in medication use to when states implemented the various policies. The findings were produced at the county level, taking into account local factors that may influence prescribing this drug.
The researchers discovered that the nationwide use of buprenorphine increased dramatically during the study period. Buprenorphine treatment months per 1,000 patients grew from 1.5 in 2006 to 22.8 in 2018.
During this time period, mandatory instruction for buprenorphine prescribers beyond the first training required for a waiver was related with significant increases in the number of months of buprenorphine treatment per individual in the year following policy implementation.
Buprenorphine use increased by around 9 treatment months per 1,000 persons in the first year, rising to more than 14 months of therapy per 1,000 people in the fifth year after adoption.
Increases were also linked to requiring continuing medical education related to substance abuse or addiction for physician license. Under such rules, buprenorphine use grew by around 7 treatment months per 1,000 people in the first year, rising to more than 11 months of treatment per 1,000 people in the fifth year.
The study discovered no link between buprenorphine dispensing and prescription drug monitoring systems, pain management clinic laws, or Medicaid rules.
“Our findings suggest that requiring education for buprenorphine prescribers and training in substance use disorder treatment for medical providers are actionable proposals for increasing buprenorphine utilization and ultimately serving more patients,” said Stein, who is director of the RAND-USC Schaeffer Opioid Policy Tools and Information Center.
“The potential benefits of training on the treatment of patients with substance use disorders is particularly important given the requirement for such training for most prescribing clinicians in the recently passed federal Consolidated Appropriations Act.”
more recommended stories
 Prenatal Smoking Raises Risk of Child Mental Disorders
Prenatal Smoking Raises Risk of Child Mental DisordersKey Summary Prenatal smoking is associated.
 Physical Activity Guidelines Gap: Walking is Insufficient
Physical Activity Guidelines Gap: Walking is InsufficientQuick Summary Walking remains the most.
 Breast Cancer Risk Rises with Aging Tissue Changes
Breast Cancer Risk Rises with Aging Tissue ChangesKey Highlights A 3-million-cell atlas reveals.
 Type 2 Diabetes Risk Rising in Genetically Susceptible
Type 2 Diabetes Risk Rising in Genetically SusceptibleQuick Summary Rising type 2 diabetes.
 Female Microbiome Shaped by Diet, Stress, Unhealthy Lifestyle
Female Microbiome Shaped by Diet, Stress, Unhealthy LifestyleQuick Summary Lifestyle factors significantly influence.
 Transcatheter Valve-in-Valve Improves Mitral Outcomes
Transcatheter Valve-in-Valve Improves Mitral OutcomesKey Highlights Transcatheter mitral valve-in-valve (mVIV).
 Stroke Rehabilitation: Early High-Intensity Therapy Findings
Stroke Rehabilitation: Early High-Intensity Therapy FindingsKey Highlights High-intensity therapy within 2.
 TRPM8 Cold Sensation Mechanism Explained for Pain Care
TRPM8 Cold Sensation Mechanism Explained for Pain CareQuick Summary TRPM8 ion channel converts.
 Gum Recession from Snus Confirmed, Caries Risk Debated
Gum Recession from Snus Confirmed, Caries Risk DebatedKey Highlights Snus use is strongly.
 Hypertensive Disorders of Pregnancy: Role of Daily Activity
Hypertensive Disorders of Pregnancy: Role of Daily ActivityKey Points Summary Limiting sedentary time.

Leave a Comment