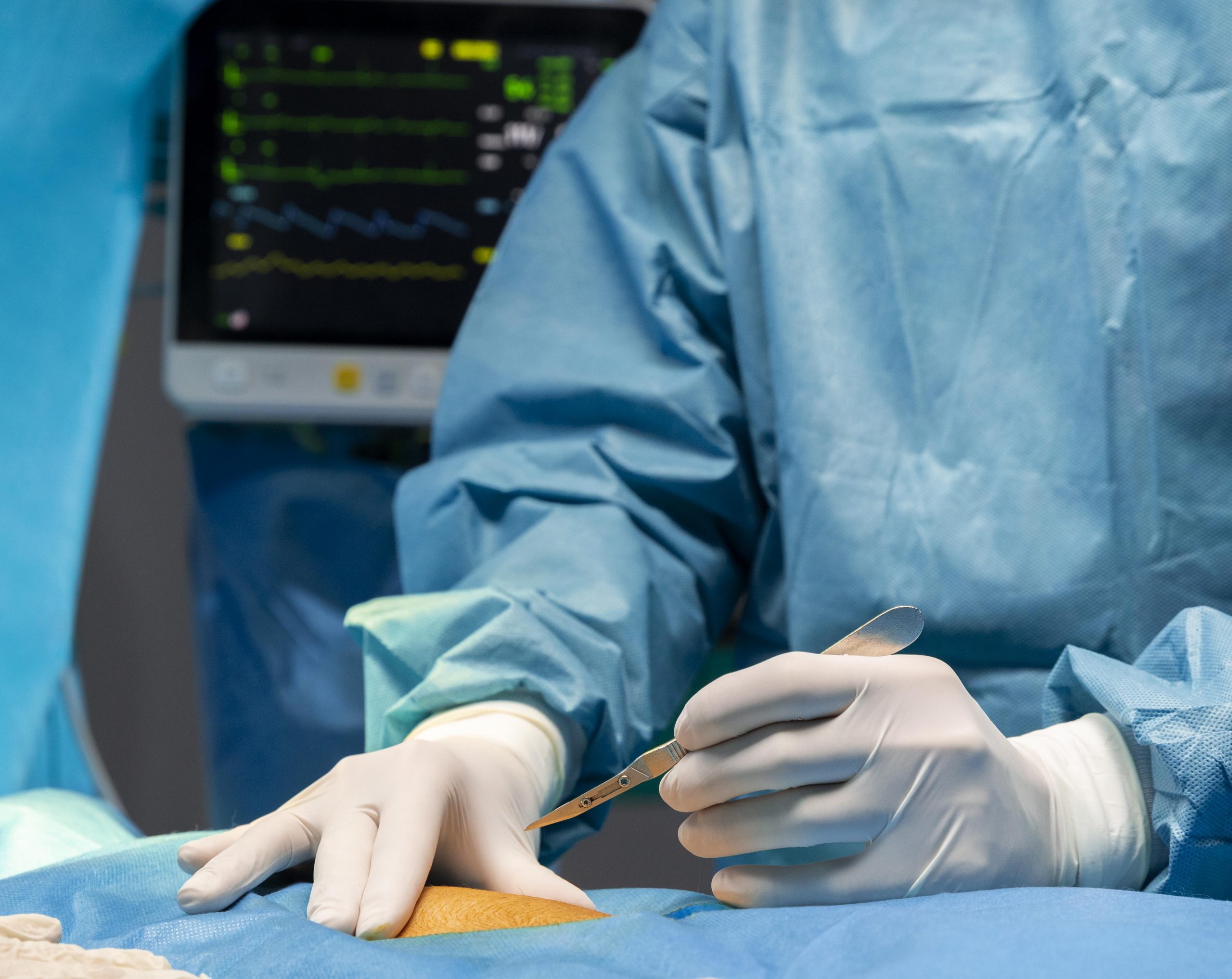

Because of the opioid crisis, doctors are less likely to give painkillers to patients to help them control their pain, even in the operating room.
A recent study published in JAMA Surgery by researchers at Massachusetts General Hospital (MGH) suggests that restricting the use of opioids during surgery may be doing more damage than good.
Researchers evaluated data on 61,249 patients who had surgery at MGH between 2016 and 2020 for the study. Patients who received more fentanyl and hydromorphone during surgery were less likely to suffer pain and required fewer opioids after waking up from anesthesia.
Furthermore, patients exposed to higher doses of fentanyl were less likely to experience uncontrolled pain or new chronic pain diagnosed within 3 months of surgery; they were less likely to be prescribed opioids at 30, 90, and 180 days after surgery; and they were less likely to develop new persistent opioid use, all with no increase in adverse effects.
“Our analysis adjusts for many factors that might influence the decision to give opioids intraoperatively, and accounts for the known properties of the drugs. Because of this we feel confident that the opioid exposure during surgery is driving this result,” says co-first author Ran Liu, Ph.D., a research fellow in the Department of Anesthesia, Critical Care, and Pain Medicine at MGH.
The findings emphasize the need of ensuring that patients do not awaken from general anesthesia in pain, not just for their immediate well-being but also to prevent persistent pain and the necessity for long-term opiate use.
“The opioid crisis is a major motivator for mitigating the risks of opioid usage,” says co-first author Laura A. Santa Cruz Mercado, MD, anesthesiology resident in the Department of Anesthesia, Critical Care, and Pain Medicine at Beth Israel Deaconess Medical Center and former research fellow in the Department of Anesthesia, Critical Care, and Pain Medicine at MGH. “But appropriate opioid administration in the operating room may reduce total opioid usage after surgery.”
Patrick L. Purdon, Ph.D., the Nathaniel M. Sims Endowed Chair in Anesthesia Innovation and Bioengineering at MGH and an associate professor of Anesthesia at Harvard Medical School, a co-senior author, stresses that more study is needed to provide more explicit direction to surgical teams.
“We need to develop new technologies to help anesthesiologists titrate and optimize opioid administration in the operating room in a personalized way,” he says. “But this data gives us evidence that such efforts could have significant long-term benefits.
more recommended stories
 One Health Summit: WHO Leads Global Health Response
One Health Summit: WHO Leads Global Health ResponseKey Highlights Global leaders convened in.
 Prenatal Smoking Raises Risk of Child Mental Disorders
Prenatal Smoking Raises Risk of Child Mental DisordersKey Summary Prenatal smoking is associated.
 Physical Activity Guidelines Gap: Walking is Insufficient
Physical Activity Guidelines Gap: Walking is InsufficientQuick Summary Walking remains the most.
 Breast Cancer Risk Rises with Aging Tissue Changes
Breast Cancer Risk Rises with Aging Tissue ChangesKey Highlights A 3-million-cell atlas reveals.
 Type 2 Diabetes Risk Rising in Genetically Susceptible
Type 2 Diabetes Risk Rising in Genetically SusceptibleQuick Summary Rising type 2 diabetes.
 Female Microbiome Shaped by Diet, Stress, Unhealthy Lifestyle
Female Microbiome Shaped by Diet, Stress, Unhealthy LifestyleQuick Summary Lifestyle factors significantly influence.
 Transcatheter Valve-in-Valve Improves Mitral Outcomes
Transcatheter Valve-in-Valve Improves Mitral OutcomesKey Highlights Transcatheter mitral valve-in-valve (mVIV).
 Stroke Rehabilitation: Early High-Intensity Therapy Findings
Stroke Rehabilitation: Early High-Intensity Therapy FindingsKey Highlights High-intensity therapy within 2.
 TRPM8 Cold Sensation Mechanism Explained for Pain Care
TRPM8 Cold Sensation Mechanism Explained for Pain CareQuick Summary TRPM8 ion channel converts.
 Gum Recession from Snus Confirmed, Caries Risk Debated
Gum Recession from Snus Confirmed, Caries Risk DebatedKey Highlights Snus use is strongly.

Leave a Comment