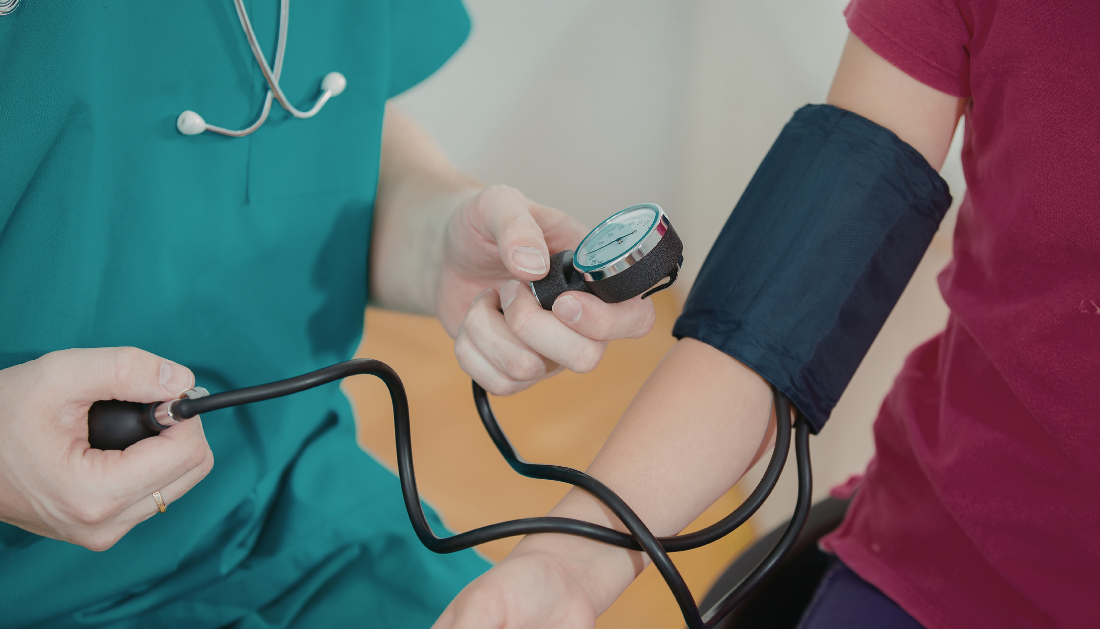

Key Takeaways
- Hypertension thresholds shifted from 140/90 to 130/80 mmHg
- Intensive control (<120 systolic) reduces CV events and mortality
- Emerging evidence links Blood Pressure control with reduced Dementia risk
- Home BP monitoring is now strongly recommended
- Clinical decisions must balance benefits vs. fall risk in older adults
Why Blood Pressure Targets Are Changing
A 78-year-old patient treated by geriatrician Mark Supiano highlights a growing clinical dilemma. Despite antihypertensive therapy, her BP remained elevated at 148/86 mmHg. Lifestyle factors, including NSAID use, sodium intake, alcohol consumption, and inactivity, contributed to poor control.
Even after improvements brought her systolic BP to 130–140 mmHg, newer guidelines from the American Heart Association and American College of Cardiology reclassified this range as hypertension.
This shift reflects a broader clinical question: How aggressively should clinicians lower blood pressure, particularly in older adults?
Evidence Driving Lower Targets
The landmark SPRINT trial reshaped hypertension management. It demonstrated that targeting <120 mmHg systolic significantly reduced:
- Cardiovascular events
- Stroke risk
- All-cause mortality
More recent studies extend these findings, showing potential cognitive benefits. Lower BP levels may delay progression of cognitive decline, reinforcing the principle: cardiovascular health supports brain health.
However, risks remain. Overcorrection can lead to Hypotension, increasing the risk of dizziness, syncope, and falls, particularly in older adults.
Balancing Benefits and Risks of Blood Pressure in Clinical Practice
Updated guidelines now recommend:
- <120 mmHg systolic for high-risk patients
- Consideration of similar targets even in moderate-risk groups
Importantly, evidence indicates that even adults aged>75 years benefit from tighter control without increased fall risk compared with standard therapy.
Explore all Cardiology CME Conferences & Online Courses 2026
Yet, not all experts fully align. Some clinicians advocate a more individualized approach, particularly for frail patients, those with comorbidities, or limited life expectancy.
Time-to-benefit is also critical. Data suggest that preventing one stroke may take nearly 1.7 years of intensive treatment in 200 patients, highlighting the need for personalized risk assessment.
Practical Recommendations for HCPs
- Encourage home blood pressure monitoring to reduce variability and white-coat effect
- Prioritize lifestyle modification alongside pharmacotherapy
- Use shared decision-making, especially in older adults
- Focus on patient-specific goals, not just numeric targets
As hypertension remains largely asymptomatic yet undertreated, these evolving guidelines call for more proactive, but cautious management.
Source:
more recommended stories
 Heart Attack Recovery: Single Injection May Heal the Heart
Heart Attack Recovery: Single Injection May Heal the HeartKey Points Researchers have developed a.
 Statins Rarely Cause Side Effects, Large Trials Show
Statins Rarely Cause Side Effects, Large Trials ShowKey Points at a Glance Large.
 New Insights Into Immune-Driven Heart Failure Progression
New Insights Into Immune-Driven Heart Failure ProgressionKey Highlights (Quick Summary) Progressive Heart.
 Population Genomic Screening for Early Disease Risk
Population Genomic Screening for Early Disease RiskKey Takeaways at a Glance Population.
 Durvalumab in Small Cell Lung Cancer: Survival vs Cost
Durvalumab in Small Cell Lung Cancer: Survival vs CostKey Points at a Glance Durvalumab.
 Vagus Nerve and Cardiac Aging: New Heart Study
Vagus Nerve and Cardiac Aging: New Heart StudyKey Takeaways for Healthcare Professionals Preserving.

Leave a Comment