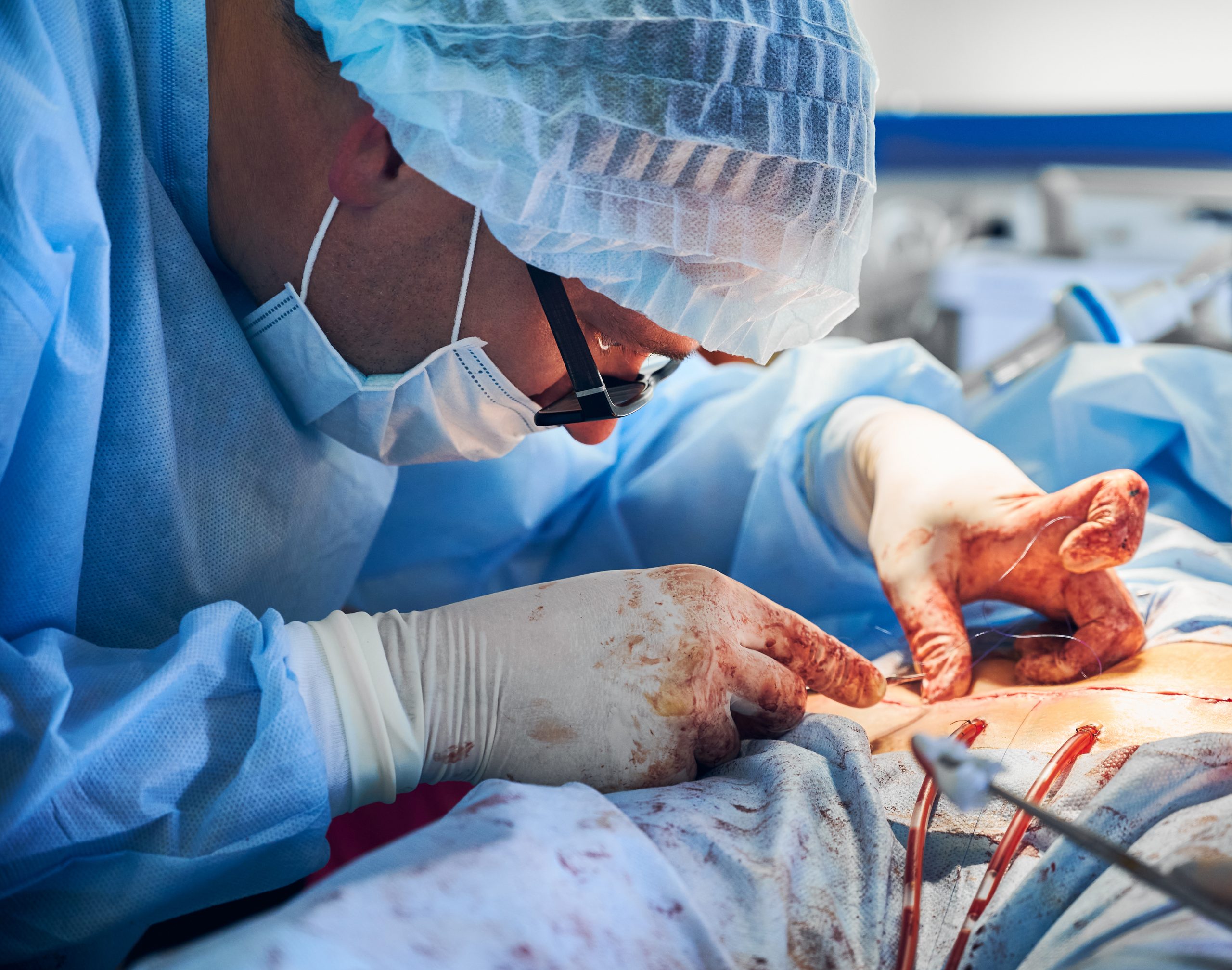

A little technical adjustment to keyhole surgery for prostate cancer has been demonstrated by German surgeons to more than halve one of the most frequent postoperative complications—lymphatic fluid accumulating in the pelvis.
The procedure entails cutting a little flap out of the peritoneum, the lining of the abdomen, and securing it into the pelvis. As a result, lymphatic fluid has a way to exit the pelvis and enter the belly, where it can be absorbed more readily.
The research results are announced during the annual European Association of Urology Conference in Milan in 2023.
Almost 10% of patients who undergo robot-assisted keyhole surgery to remove their lymph nodes and prostate cancer need to be treated for symptoms brought on by lymphocele, a condition where lymphatic fluid collects in the pelvis. When patients were routinely examined without them reporting symptoms, over a third of them were found to have lymphocele.
Superinfection, pelvic pain, pressure on the bladder, and swollen legs from vein compression are all symptoms. Symptomatic lymphocele can cause major infections or deep vein thrombosis if it is not addressed.
Treatment is complete after the fluid is no longer accumulating after three days to three weeks of draining a lymphocele. This necessitates an overnight hospital stay for certain patients.
Urology specialist Manuel Neuberger from University Medical Center Mannheim and Heidelberg University said, “When they’ve only just returned home following a cancer operation, the last thing patients need is to return to the hospital with this kind of complication, which unfortunately is fairly common. If drainage doesn’t cure the problem, then—in rare cases—the final treatment is to create an artificial opening in the peritoneum, which provides a route out for the lymph so it’s no longer stuck in the pelvis. As it’s such a simple step, why not create a flap as a standard, to prevent the condition in the first place?
“Previous studies of the technique have been inconclusive, so we designed a larger, more robust trial to ensure our findings were statistically significant.”
At University Medical Center Mannheim, the trial included over 550 patients and four different surgeons. Surgeons were not informed of a patient’s decision to have a peritoneal flap until the remainder of the procedure was complete. Also, patients were randomly assigned to one of the two groups—with a flap or without—while taking into account additional elements that could raise the risk of lymphoceles, such as diabetes, the degree of lymph node removal, the use of anti-coagulants, and the surgeon performing the procedure. Following surgery, the patients were monitored for six months.
Just 10 patients in the peritoneal flap group, as opposed to 25, had a symptomatic lymphocele by the end of the six-month follow-up period. In comparison to 46 patients in the control group, 20 patients in the flap group had lymphocele at the time of discharge but no symptoms. This increased to just 27 in the flap group during the follow-up, but 74 in the control group.
Professor Philip Nuhn, Professor of Urology at University Medical Center Mannheim, who led the research, said, “Using the peritoneal flap reduced the incidence of lymphocele from nine percent to less than four percent. We now use this as the new standard in Mannheim, and hope that—following these results—it will become common practice elsewhere as well.”
Professor Jochen Walz, from the EAU Scientific Congress Office and the Institut Paoli-Calmettes Cancer Center in Marseille said, “Most problems in these operations are linked to the lymph node removal, rather than the prostate surgery itself. Removal of the lymph nodes allows us to see if cancer has spread, so it’s important to do, particularly as surgery is now mainly used in higher-risk patients. Creating a peritoneal flap is a simple, small, easy, and quick procedure that takes about five minutes to complete. It is totally safe and this trial has shown it can substantially reduce complications, so there’s no reason why surgeons should not now do this as standard.
“Randomized control trials to evaluate technical changes in surgery are notoriously difficult to do—but this study has shown that they are both possible and effective. That’s good news for surgeons and for patients, who will benefit from better outcomes as a result.”
more recommended stories
 Phage Therapy Study Reveals RNA-Based Infection Control
Phage Therapy Study Reveals RNA-Based Infection ControlKey Takeaways (Quick Summary) Researchers uncovered.
 Safer Allogeneic Stem Cell Transplants with Treg Therapy
Safer Allogeneic Stem Cell Transplants with Treg TherapyA new preclinical study from the.
 AI in Emergency Medicine and Clinician Decision Accuracy
AI in Emergency Medicine and Clinician Decision AccuracyEmergency teams rely on rapid, accurate.
 Innovative AI Boosts Epilepsy Seizure Prediction by 44%
Innovative AI Boosts Epilepsy Seizure Prediction by 44%Transforming Seizure Prediction in Epilepsy Seizure.
 Hypnosis Boosts NIV Tolerance in Respiratory Failure
Hypnosis Boosts NIV Tolerance in Respiratory FailureA New Approach: Hypnosis Improves NIV.
 Bee-Sting Microneedle Patch for Painless Drug Delivery
Bee-Sting Microneedle Patch for Painless Drug DeliveryMicroneedle Patch: A Pain-Free Alternative for.
 AI Reshapes Anticoagulation in Atrial Fibrillation Care
AI Reshapes Anticoagulation in Atrial Fibrillation CareUnderstanding the Challenge of Atrial Fibrillation.
 Hemoglobin as Brain Antioxidant in Neurodegenerative Disease
Hemoglobin as Brain Antioxidant in Neurodegenerative DiseaseUncovering the Brain’s Own Defense Against.
 Global Data Resource for Progressive MS Research (Multiple Sclerosis)
Global Data Resource for Progressive MS Research (Multiple Sclerosis)The International Progressive MS Alliance has.
 AI Diabetes Risk Detection: Early T2D Prediction
AI Diabetes Risk Detection: Early T2D PredictionA new frontier in early diabetes.

Leave a Comment