
Key Points Summary
- Solid organ transplant recipients face significantly higher skin cancer risk due to immunosuppressive therapy
- Screening participation varies widely despite guideline recommendations
- Squamous cell carcinoma risk increases up to 250-fold post-transplant
- Barriers exist at the patient, clinician, and healthcare system levels
- Regular full skin examinations remain essential for early detection
- For More Updates on Skin Cancer and women’s health, register for #HerHealth2026
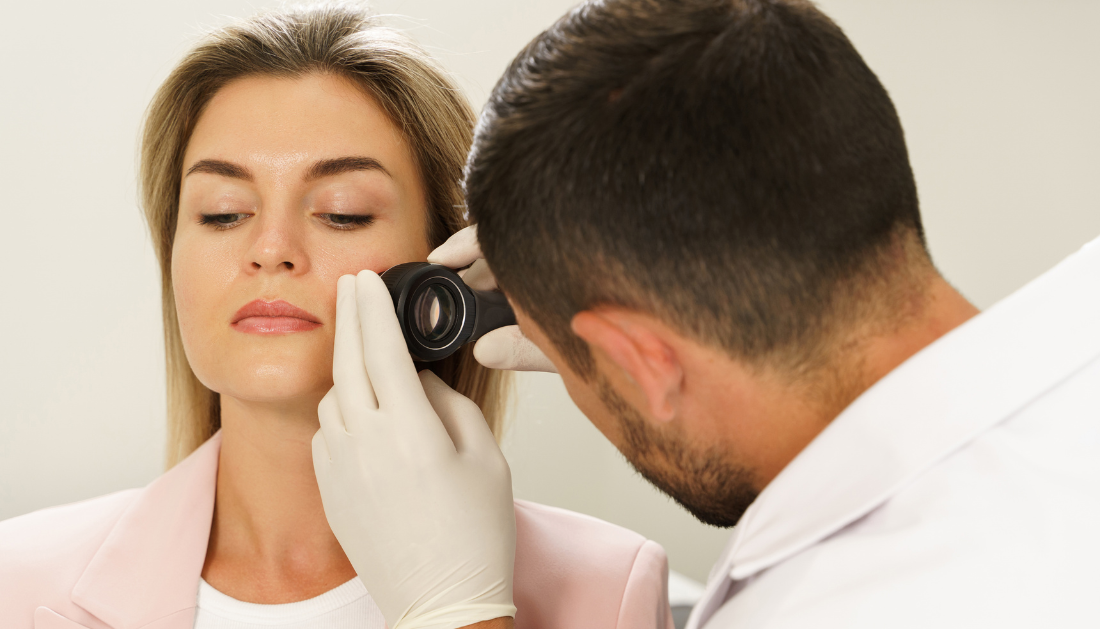
Why Skin Cancer Screening Matters After Transplant
Skin cancer screening in organ transplant patients continues to show inconsistent uptake, despite clear evidence of elevated malignancy risk. Solid organ transplant recipients require lifelong immunosuppressive therapy, which significantly increases susceptibility to cutaneous cancers.
A narrative review of 17 studies highlights a clear gap between guideline recommendations and real-world practice: annual full skin examinations for transplant recipients are not consistently performed across regions. Non-melanoma skin cancers remain the most common complication post-transplant, especially in fair-skinned populations. Compared to the general population, recipients face a 65–250-fold higher risk of squamous cell carcinoma and a 10–16-fold higher risk of basal cell carcinoma, with squamous cell carcinoma showing greater aggressiveness, recurrence, metastasis, and mortality. Melanoma risk is also elevated, reaching up to tenfold higher in some groups.
What Drives Inconsistent Skin Cancer Screening Uptake?
The variability in screening participation stems from multiple interconnected factors. Researchers categorize these into patient-level, clinician-level, and system-level barriers.
- Patient-level factors include socioeconomic status, education, and awareness of cancer risk
- Clinician-level gaps involve limited familiarity with dermatology screening guidelines and competing priorities in post-transplant care
- System-level challenges include restricted access to dermatologists and the absence of structured screening protocols
This multidimensional issue underscores that low screening rates are not solely due to patient behavior. Instead, they reflect broader inefficiencies in the coordination of care delivery among transplant teams, primary care providers, and dermatology specialists.
Strengthening Screening Pathways for Better Outcomes
Full skin examinations conducted by clinicians remain central to reducing morbidity in this high-risk group. Alongside photoprotection strategies and self-skin assessments, early detection enables timely intervention and improves outcomes.
Advanced skin cancer treatment in transplant recipients is often complex due to drug interactions and potential graft rejection risks, making prevention and early diagnosis even more critical.
Explore All Oncology CME Conferences and Online Courses 2026
The findings call for standardized screening pathways, improved risk stratification, and timely dermatology referrals. Strengthening interdisciplinary collaboration can help ensure consistent surveillance and reduce preventable complications in transplant populations.
Source:
more recommended stories
 Polygenic Risk Scores Improve Early Heart Disease Detection
Polygenic Risk Scores Improve Early Heart Disease DetectionKey Points A new multicondition polygenic.
 Prenatal Sedatives Psychiatric Risk: New Study Findings
Prenatal Sedatives Psychiatric Risk: New Study FindingsQuick Summary A large South Korean.
 Cardiovascular Health from Early Life Lowers Disease Risk
Cardiovascular Health from Early Life Lowers Disease RiskKey Points Summary: Cumulative cardiovascular health.
 Early Autism Detection Using Wearable Sensors in Infants
Early Autism Detection Using Wearable Sensors in InfantsKey Highlights: Wearable movement sensors may.
 Breast Cancer Risk via Cell Squeezing Technology
Breast Cancer Risk via Cell Squeezing TechnologyKey Highlights Novel cell-squeezing technology assesses.
 Alzheimer’s Disease Driven by Cancer Gene Mutations
Alzheimer’s Disease Driven by Cancer Gene MutationsKey Highlights Microglial cells in Alzheimer’s.
 Nivolumab Reduces Oral Cancer Risk in Phase I Trial
Nivolumab Reduces Oral Cancer Risk in Phase I TrialKey Highlights Intralesional nivolumab reduced lesion.
 Cardiovascular Risk Rises with Heatwaves Over 38°C
Cardiovascular Risk Rises with Heatwaves Over 38°CKey Highlights Extreme heat (>38°C) significantly.
 Psychedelic Use Linked to Major Life Changes Study
Psychedelic Use Linked to Major Life Changes StudyQuick Summary 83% of users reported.
 Brain Categorization Redefined by New Neuroscience Study
Brain Categorization Redefined by New Neuroscience StudyKey Highlights Brain Categorization is not.

Leave a Comment