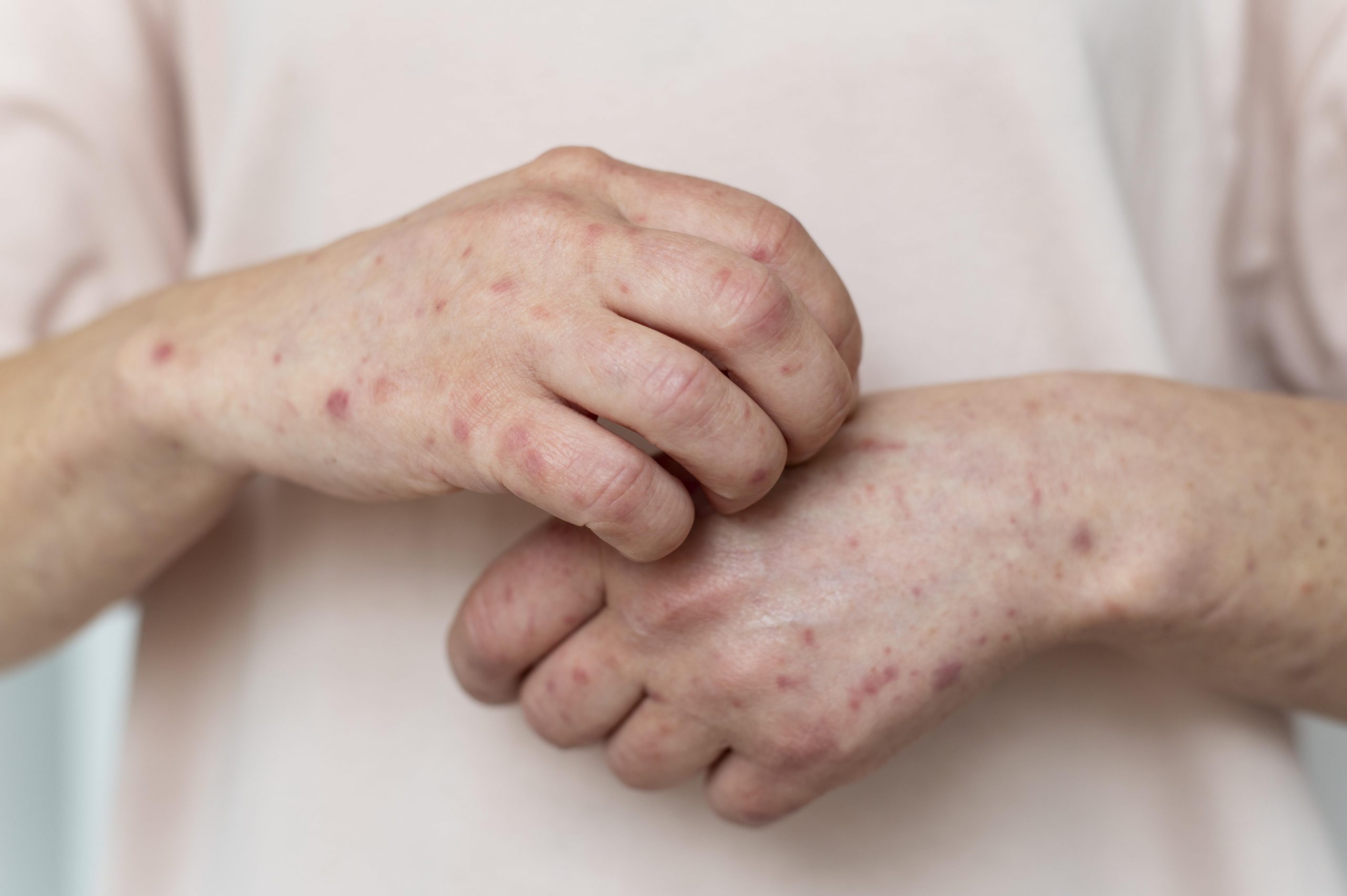

Tinea is a common, highly contagious illness of the skin, hair, or nails that is caused by molds called dermatophytes. In South Asia, a new dermatophyte species called Trichophyton indotineae has spread quickly and caused an outbreak of severe tinea that is resistant to antifungals. This epidemic is likely caused by the misuse and overuse of topical antifungals and corticosteroids. T. indotineae infections are very contagious and cause itchy, red patches all over the body (tinea corporis), the crural fold, the pubic area, and the thigh next to it (tinea cruris), or the face (tinea faciei). T. indotineae is often resistant to terbinafine, which is a standard treatment for tinea. Infections with T. indotineae have been found all over Asia, Europe, and Canada, but not yet in the United States.
On February 28, 2023, a dermatologist in New York City told public health officials that two of his patients had serious tinea that didn’t get better with oral terbinafine treatment. This made public health officials worried about a possible T. indotineae infection, even though these patients didn’t share any epidemiologic links. A clinical laboratory had already determined that the skin culture isolates from each patient were Trichophyton mentagrophytes. The isolates were then sent to the Wadsworth Center at the New York State Department of Health for further review and analysis. The isolates were found to be T. indotineae after Sanger sequencing of the internal transcribed spacer region of the ribosomal gene and phylogenetic analysis in March 2023. The CDC looked over the activities connected to this investigation and made sure they were done in line with federal law and CDC policy.
Patient A, a 28-year-old woman, had a broad itchy rash in the summer of 2021. In December 2021, when she was in her third stage of pregnancy, she saw a dermatologist for the first time. She didn’t have any other health problems, and she hadn’t been around anyone with a similar disease or traveled abroad recently. Dermatologists saw large, circular, scaly, itchy plaques on the neck, belly, pubic area, and buttocks. She was told she had tinea and started taking terbinafine by mouth in January 2022, after her baby was born. After two weeks of treatment, her rashes didn’t get better, so she stopped taking terbinafine and started taking itraconazole. After taking itraconazole for 4 weeks, the rash went away totally. However, she is still being watched to see if the infection comes back and if she needs to take itraconazole again.
Patient B, a 47-year-old woman with no big health problems, got a rash that itched all over her body while she was in Bangladesh in the summer of 2022. There, she was treated with creams that had both antifungal and antibiotic ingredients. The doctor also told her that other people in her family had similar outbreaks. After she got back to the U.S., she went to the emergency room three times in the fall of 2022. She was given hydrocortisone 2.5% lotion, diphenhydramine, clotrimazole cream (during the second visit), and terbinafine cream (during the third visit), but the rash didn’t get better. In December 2022, dermatologists checked her out and found many small, scaly, ring-shaped, itchy plaques on her legs and buttocks. She took terbinafine by mouth for 4 weeks, but her symptoms did not get better. She then got griseofulvin treatment for 4 weeks, which helped her feel about 80% better. Itraconazole therapy is being thought about until more tests are done. This is because a possible T. indotineae infection was recently confirmed. Her son and husband, who live in the same house and say they have had similar eruptions, are being looked at right now.
Several important things can be learned from what happened to these two people. Patient A hadn’t been out of the country recently, which suggests that T. indotineae could have been spread in the United States. When a patient has broad tinea, especially when the outbreaks don’t get better with first-line topical antifungal agents or oral terbinafine, a doctor should think about a T. indotineae infection. Most clinical labs that use culture-based methods to identify organisms often mistake T. indotineae for T. mentographytes or T. interdigitale. Genomic sequencing is the only way to correctly identify organisms. If a health care provider thinks a patient has T. indotineae infection, they should call their state or local public health department for help with testing. Testing is available at some public health laboratories and specialized academic and commercial laboratories. Antifungal triazole itraconazole has been shown to work when taken by mouth. But providers should be aware of problems with itraconazole absorption, which can lead to different levels of the drug in the blood; itraconazole’s interactions with other drugs; the need for treatment for up to 12 weeks; and the known rise of triazole resistance. Antimicrobial stewardship is important to stop people from misusing or overusing antifungal drugs and corticosteroids that are recommended or sold over-the-counter. Also, health care workers can teach their patients how to stop the dermatophytes that cause tinea from spreading.Lastly, public health monitoring and more testing could help find T. indotineae and keep track of its spread.
more recommended stories
 CDC Nutrition Biomarkers Study Offers Public Health Insights
CDC Nutrition Biomarkers Study Offers Public Health InsightsKey Points The upcoming CDC Nutrition.
 Macrophages Attack Live Melanoma Cells in Real Time
Macrophages Attack Live Melanoma Cells in Real TimeKey Takeaways Researchers at the Garvan.
-
Casino en el bolsillo: disfrutar el ocio de azar desde el móvil con sentido
Diseño y navegación pensados para la.
 Facial Micromovements Linked to Accurate Pain Detection
Facial Micromovements Linked to Accurate Pain DetectionKey Takeaways Researchers at Rutgers University–New.
 Ebola Outbreak in DRC and Uganda Triggers WHO Emergency
Ebola Outbreak in DRC and Uganda Triggers WHO EmergencyKey Points Summary The World Health.
 Nicotine Pouches Under Scrutiny in New WHO Warning
Nicotine Pouches Under Scrutiny in New WHO WarningKey Takeaways The World Health Organization.
 PCOS Renamed to PMOS to Reflect Broader Health Risks
PCOS Renamed to PMOS to Reflect Broader Health RisksKey Points The World Health Organization.
 Cannabis and Tobacco Co-Use May Increase Psychosis Risk
Cannabis and Tobacco Co-Use May Increase Psychosis RiskKey Takeaways A new study in.
 Walking 8,500 Steps May Prevent Weight Regain
Walking 8,500 Steps May Prevent Weight RegainKey Points A new meta-analysis presented.
 Hantavirus Cruise Ship Outbreak: WHO Issues Update
Hantavirus Cruise Ship Outbreak: WHO Issues UpdateKey Points WHO confirmed a cluster.

Leave a Comment